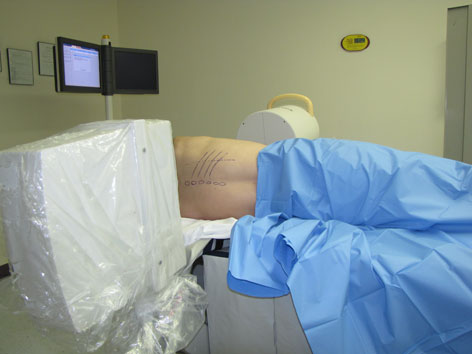
What is Kyphoplasty?
Kyphoplasty – Dr. Eduardo M. Fraifeld explains this minimally-invasive pain management procedure used to treat compression fractures of the spine.

Kyphoplasty – Dr. Eduardo M. Fraifeld explains this minimally-invasive pain management procedure used to treat compression fractures of the spine.
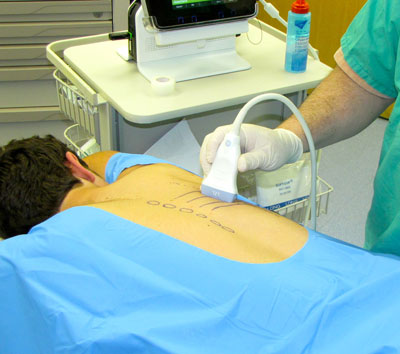


 Our treatment goals:
Our treatment goals:
You are the only one who can decide which treatment is best for you. It is important that you recognize that you have a responsibility to participate in, and take ownership of, any decisions involving your health care. You will be asked to make the final decision about what is best for you, so ask questions about anything you do not understand.
Your family and close friends are an important part of the collaborative process. We encourage you to include them in any education sessions we provide concerning your condition. If you choose to have surgery, we will make every effort to keep family members informed of your progress and to involve them in your recovery process.
Deciding which treatment option is best for you involves weighing the risks and benefits associated with each option. If you eventually choose to have surgery, your physical condition and your mental attitude will determine your body’s ability to heal. You must approach your surgery with confidence, a positive mental attitude and a thorough understanding of the anticipated outcome. You should have realistic goals — and be willing to work steadily to achieve those goals.
Angie has been working at DOC Rehabilitation since 2008. She helps with patient scheduling and billing. Angie is a graduate from Danville Community College with Associates Degree.
Diana has come back to our front office team at DOC Rehab. She has been employed since 2012 doing check-in and patient scheduling. Diana has experience in sales, customer service, and management. She graduated from the University of Tennessee at Martin with a BSBA with a major in management. Diana enjoys spending time with her friends and family while being a member of Faith Memorial Baptist Church.
Martha is the Rehabilitation Office Manager. She has been with DOC Rehabilitation since 2007. Martha has been working in billing and insurance for over 30 years.

Brittany is a Licensed Physical Therapist Assistant. She graduated from Liberty University with a BS in Exercise Science. She continued her education at Jefferson College of Health Sciences to earn her Associates Degree as a PTA. Her focus is outpatient therapy. Brittany enjoys spending time with family and outdoor activities such as kayaking, hiking, and swimming.

Chase is a Licensed Physical Therapy Assistant. He has an undergraduate degree in Health Sciences from Jefferson College of Health Sciences where he also received his PTA degree in 2018. He then went on to Liberty University to receive his Master’s in Healthcare Administration in 2021. Chase has spent time working Functional Movement Screens and is certified in FMS, SFMA, and is a certified personal trainer. Chase also has assisted in starting Spectrum’s wellness program where he spends time screening, correcting movement patterns, and implementing exercise programs for athletes, teams, and individuals. He enjoys being active and has a special interest in sports and fitness.

Aaron is a nationally Certified Athletic Trainer since 2002 and state licensed by Virginia and North Carolina. He graduated from Davis & Elkins College with a BS degree in Physical Education and Health and attained his Masters degree in Athletic Training from West Virginia University. He has certifications by JTech Medical for Functional Capacity Evaluations, FMS for the Functional Movement Screen, and is an Approved Clinical Instructor (ACI) for Averett University Athletic Training Program. Aaron also provides consulting for sports medicine to the four Pittsylvania County High Schools